Nearly 100 million Americans have obesity, and 5 to 10 million people in the U.S. are considered “morbidly” obese. Morbid obesity is usually characterized by a person being overweight by 75 to 100 pounds or more, reaching a point where the risk of developing obesity related conditions and serious diseases (co-morbidities) can lead to disability or death. Morbid obesity is also defined by having a Body Mass Index (BMI) of 40 or higher. Morbid obesity is a disease, and a chronic one – with symptoms slowly building over time.
Before Surgery
Here are some facts and statistics about obesity:
- 34 percent of adults in the U.S. are overweight, and 31 percent are considered obese
- 15 percent of adolescents and children aged 6 through 19 are considered seriously overweight
- 10 percent of children between the ages of two and five are considered seriously overweight
- The number of children who are overweight has doubled over a 30-year period
- The number of adolescents who are overweight has tripled over a 30-year period
- Each year, an estimated 300,000 deaths are linked to obesity or being overweight
- About 400,000 deaths in the year 2000 (17 percent of the U.S. total) were linked to poor diet and physical activity. This was an increase of 33 percent from 1990, accelerating the chances that lack of exercise and bad eating habits will overtake tobacco as the #1 cause of preventable death in the U.S.
Is Surgery an Option for You?
Weight loss surgery can be an effective treatment for morbid obesity and help achieve lasting results by limiting food intake and reducing appetite. To qualify for surgery you must demonstrate the following:
- Body Mass Index (BMI) of 40 or greater, with or without comorbidities (conditions such as hypertension, diabetes, sleep apnea, and/or others related to severe obesity)
- BMI greater than 35 with comorbidities
- Commitment to permanent lifestyle changes, including exercise
- Willingness to commit to treatment and long-term follow-up
- Proof that you have tried non-surgical weight loss methods and have failed to achieve significant results
- Non-smoker
- Family and social environment that is supportive
- Accepting of operative and medical risks
- Demonstrates sufficient ability to understand the surgery, potential complications, and associated lifestyle changes that will need to occur
Exclusion Criteria
- Obesity related to a metabolic or endocrine disorder.
- History of substance abuse or untreated major psychiatric disease.
- Surgery contraindicated or risks outweigh the benefits.
- Women who want to become pregnant before 18 months.
- Patient’s younger than age 16
- Patient’s older than age 60
Three Approved Surgical Options
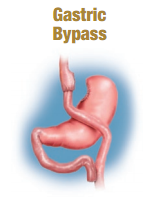
Gastric Bypass
The Roux-en-Y or gastric bypass has a long history of safety and effectiveness. It works by restricting the amount of food a patient is able to eat and decreases the amount of food that is absorbed by the intestine.
A small stomach pouch is created that holds approximately ¼ cup of intake. This limits the amount of food that can be eaten yet leaves the patient feeling full and satisfied
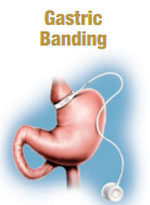
Gastric Banding
Gastric banding is a less invasive surgery that typically results in a shorter recovery time than other weight loss surgeries. A band is placed around the upper portion of the stomach. This creates a restrictive pouch that limits the amount of food that can be eaten.
Adjustments can be made to increase or decrease the band’s ability to restrict food intake. Adjustments can be made at the office; frequency depends on weight loss goals.
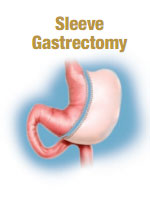
Sleeve Gastrectomy
The sleeve gastrectomy is a restrictive procedure that limits the amount of food a patient can eat, causing the patient to feel full sooner. The procedure reduces the size of the stomach by 85 percent.
Helpful Guidelines After Surgery
Following up
Follow up is an important part of any successful weight loss program. During these post-op visits, patients are educated on nutrition and the different modalities that can be used to maximize their weight loss. Furthermore, patients are also evaluated for possible malnutrition and possible cause of inadequate weight loss.

Type of Diet
After surgery, patients are expected to eat smaller meals that are high in protein, and take their daily bariatric vitamins as well as B12 supplements. In addition, they will also need to learn new eating behaviors that can help maximize weight loss without malnutrition. The following attachment will detail the dietary requirements after surgery.
Appointment request
Ask our doctor a question

How do I qualify for weight loss surgery?
You will need a BMI (Body Mass Index) of 40 without medical problems or a BMI of 35 or greater with an obesity related co-morbidity…
How much weight will I lose with surgery?
The majority of gastric band patients expect to lose 50 pounds. Patients who have sleeve gastrectomy and gastric bypass can expect to lose between 60-70% of their excess body weight.
Can I regain my weight after weight loss surgery?
Maybe. While the majority of patients will experience a life changing weight loss, some patients may not reach their weight loss goal. Diet and exercise are important components to a successful weight loss program.

